Nursing at Littleton Hospital: Through the Ages
The Littleton Hospital Association formed in 1906 with Dr. William J. Beattie as the founding doctor and a member of the Littleton Hospital Association Board of Directors. The hospital building opened in 1907. The Littleton Hospital Board of Directors appointed Miss Nellie Farr, “an experienced nurse”, as the first Superintendent of the Hospital On Wednesday, March 20, 1907. The Board described Miss Farr as “popular”, as she was “in touch with a large class, not only of our own people, but also summer residents. Her amiable disposition and tactfulness make her well fitted for the position. Miss Farr is in Boston taking a post graduate course in special work under Miss Lucy S. Drown, Superintendent of the Boston City Hospital [and Training School for Nurses].”
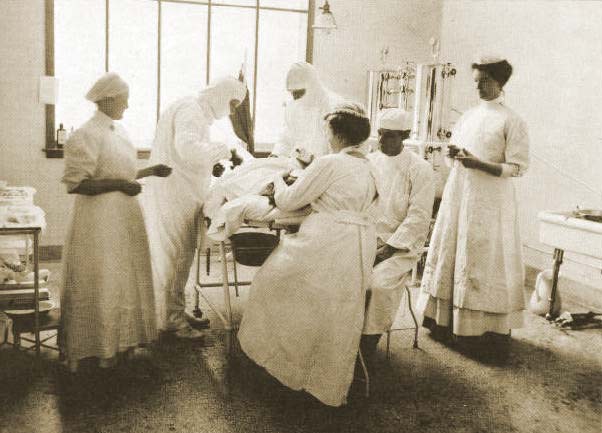
The operating room in 1907. Staff are identified as (l to r): Miss Nellie Farr, Dr. Page, Dr. Beattie, Miss Ferrin and Miss K. MacDonald
While at Boston City Hospital, Miss Farr was learning the responsibilities of a Superintendent from Miss Drown. Frances Heald, a historian from Littleton, New Hampshire reported that Dr. Beattie also had a hand in the training of Miss Farr for her responsibilities as the Hospital Superintendent. The White Mountain Republic Journal reported that on Friday, June 14, 1907 “Miss Nellie Farr, the Matron,” was present at the hospital to supervise the placement of furniture and accoutrements as they arrived. Her dedication to patients was unsurpassed. An anecdote revealed that Miss Farr once gave up her own room at the hospital to a patient! The community dedicated the hospital building on June 27, 1907. In the early days of the hospital, it was accepted practice for the Superintendent to be the Executive Officer of the hospital. The Superintendent provided direction and administrative supervision in the daily operation of the hospital while reporting to the Board of Directors. In this capacity the Superintendent was in charge of every department of the hospital. Until 1921 the Superintendent also served as the chief anesthetist. By 1915, the Board of Directors voted to make the job of treasurer a separate paid position.

In 1910, Dr. Beattie and Miss Nellie Farr created a three year nursing program that met the requirements of the NH State Board of Registration for Nurses. In this year, Dr. Beattie began in earnest to conduct the actual training of Littleton Hospital nurses. He recruited four young “ladies” from East Weymouth, Massachusetts to come to Littleton Hospital Nursing School. These first students did not need uniforms but were expected to wear “nice clean dresses each day.” Their training was mostly practical in nature. Student nurses were expected to serve night duty soon after their training began. The Board of the Littleton Hospital Association leased the nearby Lathrop House to serve as a residence for the students in nurses training.
The curriculum for the nursing program included deportment, health order and cleanliness, theory of nursing, hygiene, anatomy and physiology, dietetics, solutions, bandaging, ethics, diseases of the nervous system, materia medica (study of remedies of the eye, ear, nose and throat), contagious diseases, children’s diseases, obstetrics, bacteriology, diseases of the skin, urinalysis and massage.

In her role as Superintendent of the Hospital, Miss Nellie Farr also directed the Littleton Hospital School of Nursing from its beginning in 1910. She managed the administration and disciplining of students as well as proctoring student examinations. Miss Farr returned to private nursing duty in 1913 and Mrs. Isabel R. Jarvis, who had been Principal of the School of Housekeeping in Hartford CT, was hired as the Littleton Hospital Superintendent. Part of her job included supervising the newly expanded School of Nursing at the Littleton Hospital.
By 1918, the Board of Directors considered expanding the School of Nursing. The demand for trained nurses during World War I increased as many nurses were recruited for military service. The need to educate and train new nurses became urgent. During this period, the Trustees authorized payment of travel expenses to New York for “local ladies to study nursing”. In 1918 the Board decided to buy a neighboring residence (the Richardson House – down Cottage Street) to serve as a temporary home for the Hospital School of Nursing.
Superintendent Jarvis made several important changes in 1919. Mrs. Jarvis requested a clerical assistant. At that time a “pupil nurse” was authorized to be paid $5 per month “to keep books and records as the Superintendent required.” The hospital also hired a nurse this year to operate the x-ray machine.

In 1922, the Remich family made a donation to the hospital that enabled the Board of Trustees to authorize the construction of a larger building to house the students in the School of Nursing. It was built on land adjacent to the hospital and a tunnel was provided for access to the Hospital. When the Remich Home for Nurses was dedicated, Miss Margaret Nicholson, who was originally from Prince Edward Island (PEI), was hired as Superintendent. Miss Nicholson, known as “a most able and efficient head of our hospital,” was influential in attracting several young ladies from PEI to attend the Littleton Hospital School of Nursing. One of these students was named Sadie Miller, From Central Lot 16 on Prince Edward Island, Sadie began nurse training at Littleton Hospital on August 22, 1929.
At this time, Miss Nellie Farr became the Supervisor of the School of Nursing, overseeing the management of the Remich House. Miss Farr remained employed at the Remich House until its closure in 1935.
As a result of the economic depression that began in 1933, the hospital board had to reduce expenses. In October of 1935, the Board voted to discontinue the Littleton Hospital School of Nursing. According to the minutes of a Board meeting held at 2:00 PM October 25, 1935, recorded by B. Beattie, Secretary, “The staff of doctors is in favor of discontinuing Littleton Hospital Training School for Nurses if the Superintendent and Board of Trustees agree that such a move is advisable.” Littleton Hospital closed the Remich House and discontinued its School of Nursing in the Fall of 1935 to save the cost of fuel during the upcoming winter. Students attending the school were placed in other schools to complete their training. By this time, the Littleton Hospital School of Nursing had trained nearly 200 young women and graduated over 60 nurses.
This file [77 KB pdf] contains a list of the women who trained at Littleton Hospital’s Training School for Nurses.





In 1941, due to wartime demand, there was once again a shortage of nurses. To meet this demand, the Hospital appealed for former nurses to return on a temporary or part time basis. The Red Cross provided the Hospital with volunteers trained to serve as nurses’ aides. These assistants reduced the number of nurses needed to staff the hospital units.
In 1942, Mrs. Emma Bass became the eleventh Superintendent of the Littleton Hospital. In September of 1945 the war came to an end, and the Baby Boom began. In 1946, Mrs. Bass was quoted as saying, “Our present nursery was built to care for eight babies. We now frequently have 12-15 at a time in bureau drawers and boxes, or on radiators, sinks and tables.” The new nursery opened on January 8th, 1950, with temperature and humidity controlled by air conditioning, and 12 new bassinettes on wheels. “It means that all babies henceforth delivered in the Littleton Hospital will enjoy every known protection for survival.”
By September 14, 1948, Trustees’ minutes stated that, “Mrs. Bass mentioned that the nurses wanted holiday pay amounting to an extra day of pay for each holiday worked and that nurses generally were attempting to get their work week down to 40 hours per week.” At that time, in addition to regular pay, the Hospital paid nursing staff who did not reside in the Remich House $30 per month in addition to their regular pay.
In 1949, the Board of Trustees voted to employ a full-time business manager for the Hospital. This decision shifted all administrative duties from the Superintendent of Nurses to the business manager. The Business Manager also managed many functions of the Trustees. Emma Bass, who married Robert Straw, became Mrs. Straw and resigned in 1951. Stella Austin, who replaced Mrs. Straw, was referred to as Superintendent and more often as Director of Nurses and Nursing Services.

In 1965 the US Government passed the Medicare Act. This increased the ability of elderly citizens to pay for health care. By 1967, Littleton Hospital once again experienced a nursing shortage due to increases in the volume of patient admissions. Mr. Schauer, the Hospital Director at this time, reported that the State Division of Vocational-Technical Education agreed to underwrite a refresher course for inactive registered nurses. The State offered this course to the Hospital at no cost, as long as the Hospital provided space for a classroom. The most difficult task for this endeavor was to find an instructor for this program.
The hospital began construction of an intensive care unit (ICU) that included a cardiac care program in 1971. To meet the staffing needs of this unit, the hospital sent a team of nurses to Boston City Hospital and the Medical Center at the University of Vermont in Burlington, VT to train for the care of patients needing intensive care. Nursing shortages further strained the Hospital when the ICU opened on September 20, 1971. Staffing the ICU left a shortage of nurses on the acute care (Med-Surg) unit. The Hospital recruited more nurses through advertisements in nursing journals, the Manchester Union Leader, utilizing a nurse consultant, and publicizing vacancies at seminars and regional meetings. The hospital reduced the nursing workload by placing ward clerks on the nursing units for two shifts each day. The communication of patient care needs between nursing units was improved and weekly department head meetings addressed patient needs regularly. As the Hospital began expanding its services, administration began to question its role in the community as a “cottage hospital”. The Hospital now provided critical as well as acute care and maternal-child care services to the community. These additional services lead to a change in name that included the concept of a “regional hospital”.
Littleton Regional Hospital continued growing to keep pace with the demands of its service area and to stay competitive with current trends in healthcare. As Littleton Regional Hospital, it greatly expanded its services to provide primary and specialty care throughout the Littleton region. As a result of the increase in services, the Nursing Department has cultivated a team of nurses with credentials in such areas as emergency and critical care nursing, acute care nursing, peri-operative nursing, cardiac diagnostic lab and cardiac rehabilitation nursing, oncology/infusion therapy nursing, and maternal-child nursing, across the continuum of care.
Nursing Education expanded in a big way upon the formal affiliation of the four critical access hospitals and home health and hospice agencies in northern Grafton and Coös Counties in 2016. Littleton Regional Healthcare, Weeks Medical Center, Androscoggin Valley Hospital, Upper Connecticut Valley Hospital, and North Country Home Health/Hospice are now known as North Country Healthcare (NCH). These agencies merged their education and staff development into a system-wide department under the direction of Catherine B. Flores PhD, RN. In her role as director, Dr. Flores is standardizing staff development across all North Country Healthcare member agencies, and oversees a state of the art simulation lab at the Northwoods Center for Continuing Education in Whitefield. The Center for Learning is a hub for continuing education and professional development activities for health care professionals in the North Country, including professionals certified in pre and post-hospital care.
Though the Littleton Hospital School of Nursing closed its program in 1935, Littleton Regional Healthcare continues to play a vital role in the development of clinical nursing skills and professional development as part of the North Country Healthcare affiliation. In rural communities, the role of nursing has expanded over the last decade to include services provided by nurses who are certified in specialties such as Diabetes Education, Wound Care, Oncology, Peripherally Inserted Central-venous Catheters, Sexual Assault Nurse Examinations, and Emergency Cardiac Care. Nurses with graduate degrees provide advanced nursing practice services such as Nurse Hospitalist, Anesthesia Administration and Pain Management, Adult and Pediatric Primary Care, and Advanced Emergency/Critical Care Nursing.
To support the professional growth and development of nurses who strive to fill these roles, the North Country Healthcare system has created an environment that supports ongoing professional growth. Staff nurses are encouraged to become members of the Clinical Skills Development Team which develops and evaluates acute and critical clinical skills on the nursing units. They are prepared and certified to precept senior nursing students from local Bachelor of Science in Nursing (BSN) programs and to guide new graduate nurses through their transition from student to clinician. North Country Healthcare is a partner with White Mountain Community College, Plymouth State University, the University of New Hampshire, and the Massachusetts College of Pharmacy and Health Sciences nursing programs. These programs send nursing students to NCH member agencies for their clinical experiences. Advanced Practice nurses in North Country Healthcare supervise and evaluate graduate nursing students in Emergency Care, Women’s Health, Pediatrics, Anesthesia, and as Nurse Hospitalists from the Rivier University, University of New Hampshire, Vanderbilt University, the Kentucky Frontier School of Midwifery, Georgetown University, and Chamberlain University.
×
- Nellie Farr
- Isabel Jarvis
- Miss Baker
- Edith Bennett
- Myrtle Hallowell
- Isabel M. Hall
- Margaret Nicholson
- Georgia A. Lafferty
- Marianne Hill
- Alma Murphy
- Emma Bass
- Mrs. Robert Straw
- Stella Austin
- Alphonsine H. Hiller
- Madeline E. Plante
- Ronald Jacobus
- Evelyn Baker
- Madeline Plant (interim)
- Mrs. Savage
- Ann Wiggett
- Robert Kyle (interim)
- Richard C. McGinnis
- Lois Collins
- Isabella Garibaldi
- Linda Gilmore
- Koren Superchi
Ann C. Wiggett, R.N.
 Ann C. Wiggett was born in Plymouth, NH and grew up in West Thornton and Lincoln. She worked as a registered nurse (RN) at Littleton Hospital for 54.5 years. Right after high school, Ann went to UNH for one year. She quickly changed paths, deciding on a nursing career. She moved on to the Elliot Hospital School of Nursing, Manchester, NH, and graduated from this three-year diploma program in 1958. She received the Caritas Christi medal upon graduation which indicated she was second in the class and was “an all-around nurse.” Ann’s first year of work as an RN was in the Operating Room of the Elliot Hospital.
Ann C. Wiggett was born in Plymouth, NH and grew up in West Thornton and Lincoln. She worked as a registered nurse (RN) at Littleton Hospital for 54.5 years. Right after high school, Ann went to UNH for one year. She quickly changed paths, deciding on a nursing career. She moved on to the Elliot Hospital School of Nursing, Manchester, NH, and graduated from this three-year diploma program in 1958. She received the Caritas Christi medal upon graduation which indicated she was second in the class and was “an all-around nurse.” Ann’s first year of work as an RN was in the Operating Room of the Elliot Hospital.Ann returned to UNH in 1982, and obtained a Bachelor of Science (BS) degree in Health Administration. At Littleton Hospital Ann appreciated the influence of Evelyn Fitch who was her 3 to 11 supervisor. Evelyn set a great example to the nurses, as she thought all patients deserved “tender loving care”.
One of Ann’s fondest memories of working at Littleton Hospital was being in the OR with Dr. McDade. There were times when birds would come close enough to a window in the OR to allow identification. Dr. Harry McDade, the consummate naturalist and teacher, would teach OR staff about these birds and the finer details to distinguish one species from another. Ann also recalled Dr. McDade yelling orders during a disaster (drill) at the time when the Green Berets were training at Cannon Mountain. She was always impressed with the camaraderie and team spirit at Littleton Hospital. There was always such a willingness to help one another.
Ann witnessed many changes over the course of working at Littleton Hospital for over 54 years. When she started working at Littleton Hospital in 1959 she had to sharpen needles, wash, dry and powder gloves before sterilizing the needles, make up surgical packs, wash and sterilize surgical instruments, prep surgical patients and sometimes help with obstetrics. At that time (1959), Littleton Hospital had 49 beds, with OB, med/surg, OR, lab, x-ray, dietary and ER. When working the 3-11 shift, one medication nurse was responsible for administering medications to all patients on the one large med/surg floor – an enormous responsibility.
In 1975 a new ER was added as well as new operating rooms, new med surgery, new OB unit and a new Intensive Care Unit (ICU). At this time Ann was one of three nurses sent to Boston and Burlington to learn cardiac care in preparation for the new cardiac care unit at the hospital. Also at this time, Mary Hitchcock Hospital in Hanover, NH began sending oncology physicians for monthly clinics. As the volume of oncology patients increased, the hospital hired an oncology physician, allowing daily oncology clinics and administration of chemotherapy more frequently. The next big change came with the building of a whole new hospital in 2000 the year 2000. Keeping abreast of major changes in the healthcare industry, the new hospital has fewer beds, but far more outpatient services.
Ann would like to leave the next generation of nurses with a few thoughts that guided her through a long, rewarding career at Littleton Hospital. She thinks it is very important for nurses to carefully listen to patients. She wants today’s nurses to remember the importance of observing patients; especially in these times when so many processes are automated. She feels that TLC is essential to getting the patient out of the hospital quickly. From Ann – take the time to give back rubs, leave the call bell within reach, and be sure the patient’s water is fresh.
Source:
Interview, January, 2019
Patricia (Pat) Campbell, R.N.
 Pat Campbell worked as a registered nurse (RN) at Littleton Hospital for 24 years. She worked on both the Med Surg floor and the Cardiac Care Unit (CCU). Having lived in the North Country since 1970, Pat graduated from the Lynn Hospital School of Nursing, located in Lynn, MA in 1954. Although Pat did not originally plan for a career in Nursing, when she completed high school, her father’s health was not good. He informed Pat that she could either become a secretary or go to nursing school. Pat chose the latter, at a total cost of $200.00 for three years!
Pat Campbell worked as a registered nurse (RN) at Littleton Hospital for 24 years. She worked on both the Med Surg floor and the Cardiac Care Unit (CCU). Having lived in the North Country since 1970, Pat graduated from the Lynn Hospital School of Nursing, located in Lynn, MA in 1954. Although Pat did not originally plan for a career in Nursing, when she completed high school, her father’s health was not good. He informed Pat that she could either become a secretary or go to nursing school. Pat chose the latter, at a total cost of $200.00 for three years!Pat always looked tidy in her nurse’s cap and uniform. She was one of the last nurses who wore a white uniform at all times. According to Pat, the physicians liked to have the nurses wear their caps, as it set them apart from other staff wearing similar uniforms. Pat was a great role model for the nursing students from the Berlin Tech School (now White Mountains Community College).
The employees at Littleton Hospital were a family. In Pat’s words, “the Hospital was a community working together for the purpose of the patient. It was the people’s hospital.” She recalls working closely with Drs. Bishop, Gale, and Monroe, and the stimulating experience of rounding on patients with Dr. McDade, a wonderful teacher.
Pat’s greatest challenge of her work career was going back to school as an adult for a four-week course to learn cardiac care at the Mary Hitchcock Memorial Hospital in Hanover, NH. As Littleton opened its cardiac care unit in the early 1970’s, Pat cited how technology dramatically changed how nurses cared for patients, with the advent of cardiac monitoring; and improved diagnosis of heart conditions, combining use of the treadmill with the cardiac monitoring (known as a “stress test.”) Pat noted that Dr. Robert Gale performed the first stress test at Littleton Hospital – on himself.
Pat still lives in Littleton, NH with her husband, Tom. They are both active volunteers at Littleton Regional, and participate in many events throughout the community. Pat and Tom also enjoy visiting with family both near and far.
Toni Thomas, RN
 Toni was born in Berlin, NH, and lived in Berlin until she moved to Littleton in 1969. She attended Nursing School at the St. Louis Hospital School of Nursing in Berlin from 1964-1967. Toni Thomas worked in multiple roles as a nurse at Littleton Regional Hospital from 1970-2011. Beginning as a staff nurse on Med/Surg, she also worked in Obstetrics, Emergency Services, and ICU. She worked her way up to a nurse manager on Med/Surg, ending her career with four years in Quality Services. Toni cited that she always cared deeply about what was best for the patients, and that she was able to give them the best care possible, as Littleton Regional gave her the tools she needed to perform high quality work.
Toni was born in Berlin, NH, and lived in Berlin until she moved to Littleton in 1969. She attended Nursing School at the St. Louis Hospital School of Nursing in Berlin from 1964-1967. Toni Thomas worked in multiple roles as a nurse at Littleton Regional Hospital from 1970-2011. Beginning as a staff nurse on Med/Surg, she also worked in Obstetrics, Emergency Services, and ICU. She worked her way up to a nurse manager on Med/Surg, ending her career with four years in Quality Services. Toni cited that she always cared deeply about what was best for the patients, and that she was able to give them the best care possible, as Littleton Regional gave her the tools she needed to perform high quality work.In her retirement, she and her husband are enjoying some travel, spending time with grandchildren and having plenty of leisure time. She takes pleasure in social time with old friends and has made many new ones when interacting with her children, grandchildren, and their friends. Toni volunteers at the hospital one day a week. She is glad to be able to give back to the place that gave her so much during throughout her career.
Sources:
Boswall, EO, (1901). The Boston City Hospital Nurses’ Club, The American Journal of Nursing, 1(5), 351-354. Retrieved from jstor.org.
Colby, Jack, ed. Littleton: Crossroads of Northern New Hampshire, Town of Littleton, 1984.
Annual Report of the Trustees of the City Hospital, Boston, Issues 45-47, By Boston City Hospital. Retrieved from books.google.com.
Littleton Hospital Trustee Meeting Notes 1906-1943, Littleton Hospital Archives, Littleton, NH. Reed, Len (1981). Hospital History 1906-1981. Littleton Hospital Archives, Littleton, NH.
Interview with Frances Heald, May 1998.



